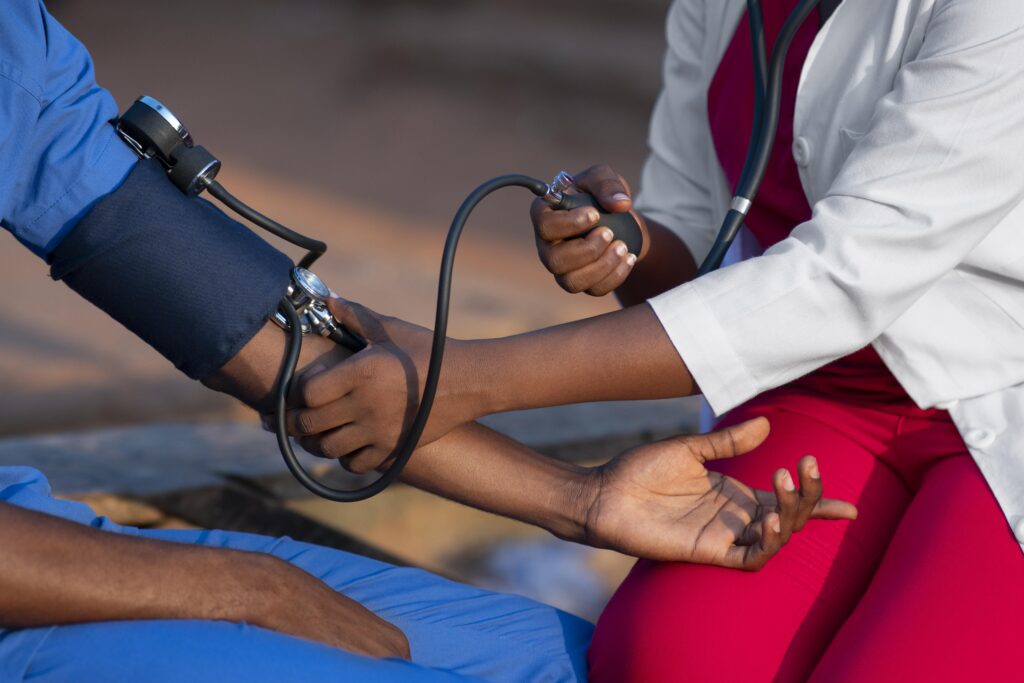
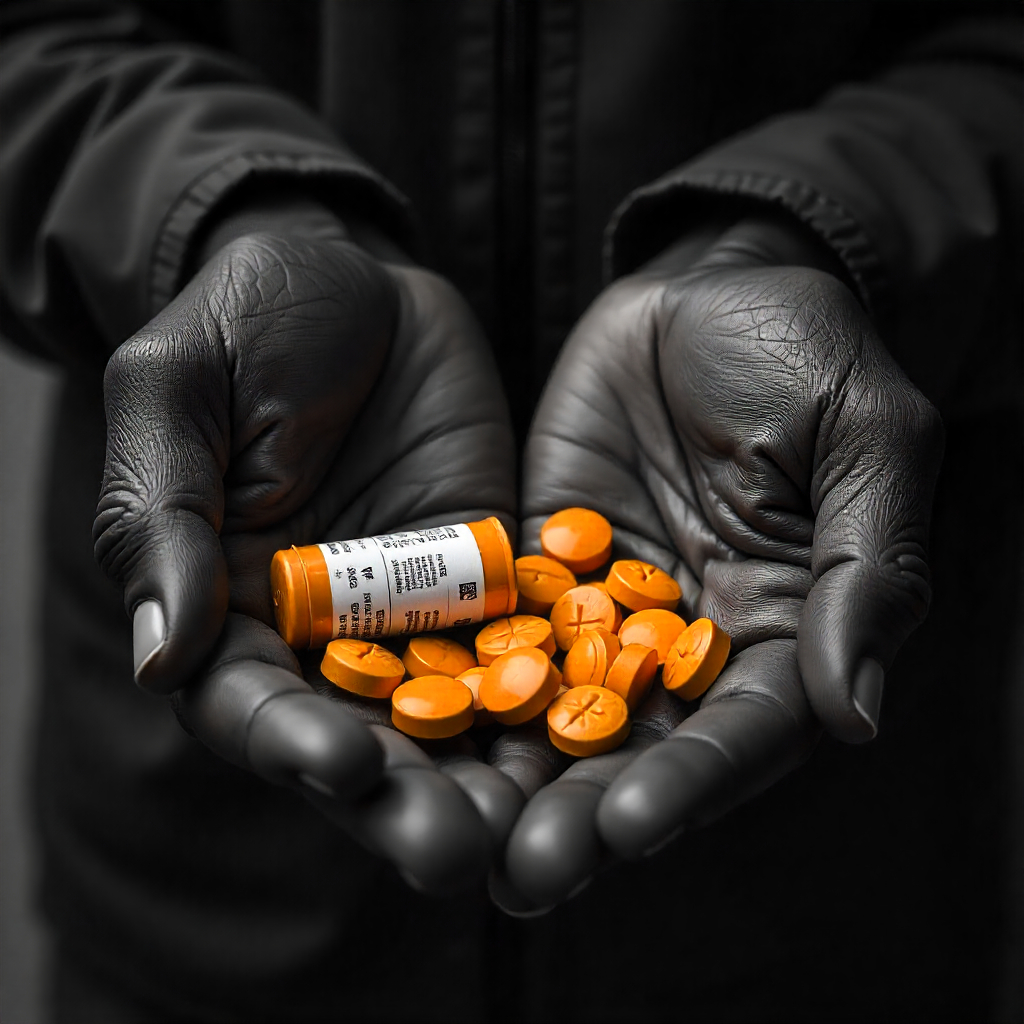
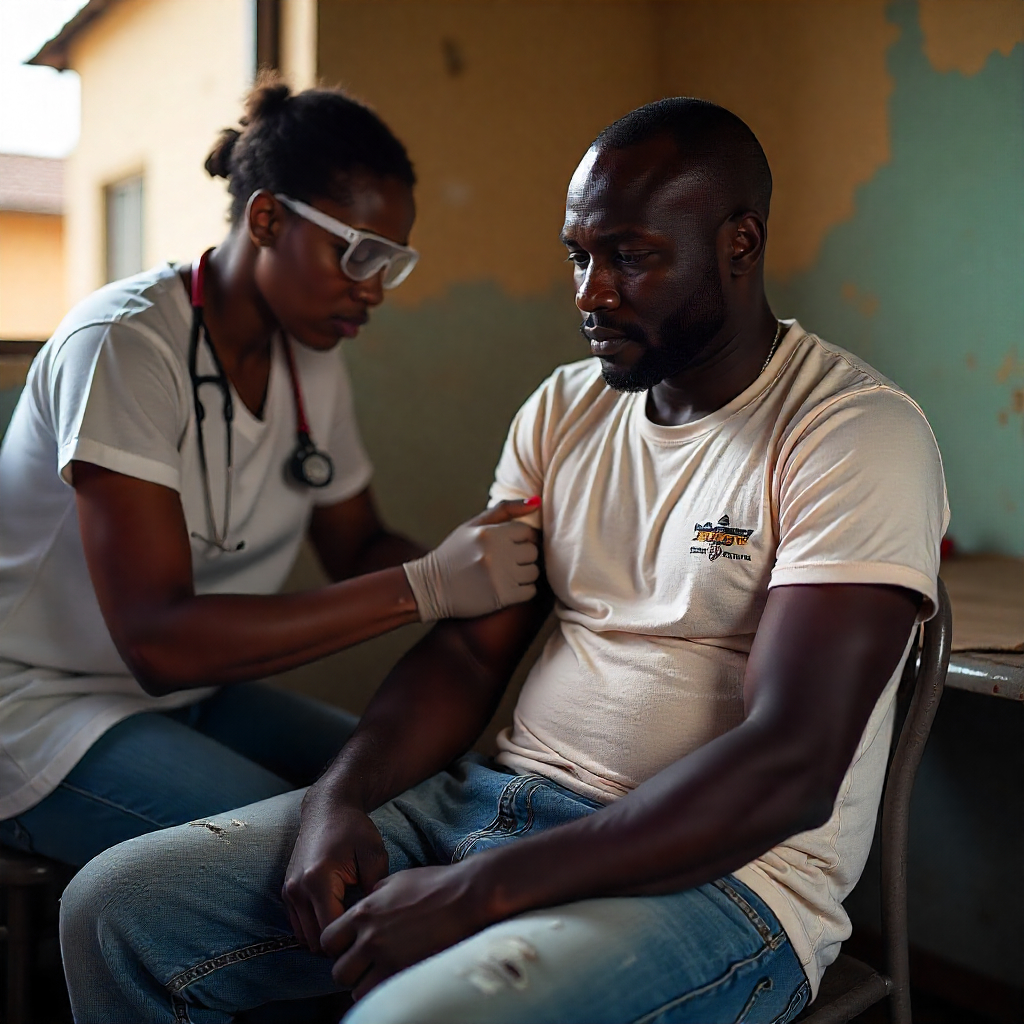
Community-Led Solutions: How African Migrant Organizations Are Addressing Healthcare Gaps Through Peer Support and Advocacy
Certainly! Here’s the revised version of your blog post with enhanced use of transition words and phrases to improve flow and coherence. Transitional elements are used to guide the reader smoothly between sections, ideas, and examples. How African Migrant Organizations Are Addressing Healthcare Gaps In a cramped Hillbrow flat in inner-city Johannesburg, Fatou*, a 29-year-old […]